Depression is one of the most common mental disorders, affecting over 300 million people around the world. It significantly contributes to morbidity and, in the US, is the number one cause of disability among individuals aged 15 to 44. Depression, which affects people of all ages, genders, and races, serves as a formidable public health concern. A combination of antidepressant medication and psychotherapy is the first line of treatment, but many individuals continue to experience symptoms of depression even after treatment. This is referred to as treatment-resistant, or refractory, depression.
Within populations of individuals with depression, almost 20% demonstrate treatment resistance. Around two-thirds of people taking their first antidepressant medication do not experience adequate symptom relief, so they are given another type. However, every subsequent medication that is tried is increasingly less effective than the one before. This has created an enormous challenge for doctors when attempting to figure out how to cure treatment-resistant depression. Because it is so difficult to manage, this type of depression has prompted other innovative methods over the years.
Along with medication and psychotherapy, doctors have found success with neuromodulation techniques, such as electroconvulsive therapy (ECT) and other brain stimulation methods, including deep brain stimulation and vagus nerve stimulation. ECT, also called shock therapy, has been utilized for decades and is considered the most effective treatment for treatment-resistant depression. Still, it can be difficult for many patients to tolerate due to its cognitive and memory side effects. A new treatment option called transcranial magnetic stimulation (TMS) has been shown to provide relief from treatment-resistant depression without ECT’s side effects.
What Is TMS?
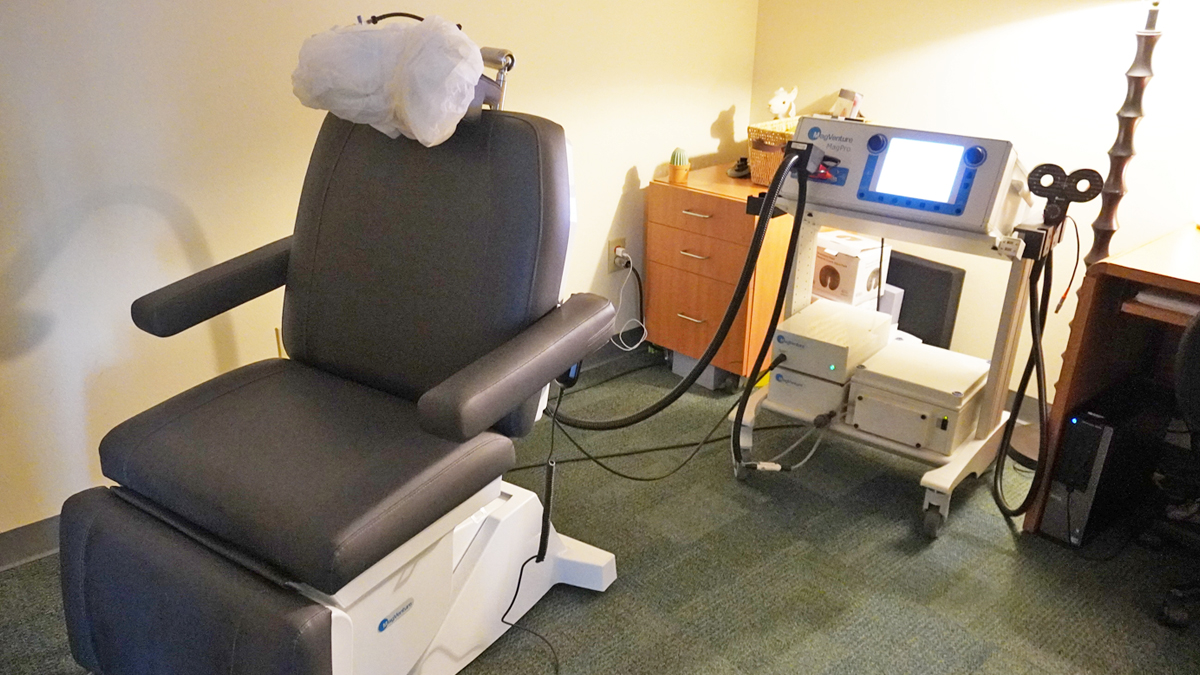
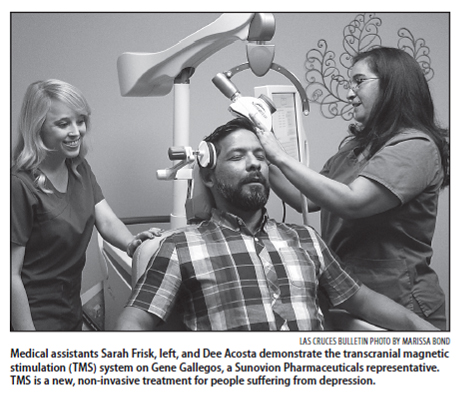
TMS is a safe, effective, non-invasive treatment method using magnetic stimulation of specific brain regions. It is one of the most advanced treatment options available today and is the only FDA-approved depression treatment that does not require medication or surgery. The TMS device transmits energy using a coil and coil generator to distribute small electric currents through the scalp and directly into specific regions of the brain. These devices were originally developed in 1985, but this technology may be traced back to the 18th century, when scientists delivered electrical stimulation to the human body to observe the effects.
TMS Therapy for Depression—How It Works
TMS therapy is conducted while the patient is awake. The clinician employs a coil to deliver magnetic stimulation to two specific parts of the brain within the frontal lobe—the motor cortex and the dorsolateral prefrontal cortex. The motor cortex is involved in the planning, execution, and control of voluntary movement. Each part of the body is connected to a specific area in the motor cortex, allowing for the integration of incoming somatosensory input with a goal-directed movement.
The prefrontal cortex is implicated in various executive functions, including focusing attention, planning for the future, predicting consequences, decision making, social cognition, and working memory. Often referred to as the seat of personality, it shapes perceptions of the self and our environment, allowing us to navigate the world around us successfully. Studies of individuals suffering from depression show decreased activity in this area.
TMS delivers magnetic pulses of the same strength as those employed by MRI machines. Also called rTMS because it uses repetitive pulses, the magnetic coil creates small electric currents that focus on and stimulate targeted brain regions while minimizing stimulation of non-targeted regions. The technician first targets the motor cortex to determine the proper anatomical area and ideal intensity of stimulation. Targeting allows technicians to discover the best location on that specific individual’s brain to place the coil and determine how much intensity it needs to fire for adequate stimulation.
After these calculations have been found, they are used to find the dorsolateral prefrontal cortex, the region showing the most robust evidence of clinical efficacy. TMS applies currents that cause the neurons to become active and release neurotransmitters but are small enough not to be felt by the patient. Repetitive treatments help your brain relieve depression symptoms by creating muscle memory that works to continue releasing these chemicals.
While the biological reasons behind why rTMS works aren’t totally understood, magnetic stimulation has shown significant effects on the brain’s functioning, alleviating symptoms of depression, and improving mood. Different ways exist to perform this procedure, and techniques of TMS therapy for depression may adapt in the future as more is learned about how to perform the treatments most effectively.
Safety and Side Effects of TMS Therapy
TMS treatment for depression is safe for most individuals, except for those with metallic items in their skulls. Unlike deep brain stimulation or vagus nerve stimulation, TMS does not necessitate implantation of electrodes or surgery of any kind. An analysis of several studies involving over 10,000 active treatments shows TMS is safe, with no adverse effects on memory or concentration, and none of the systemic side effects are linked to antidepressant medications.
Considering how effective TMS therapy is, there are very few side effects. Common side effects are usually mild to moderate, improve quickly after the end of a session, and decrease severity with subsequent sessions. The most frequently reported side effect is mild headaches or cranial pain. At the same time, other patients may experience scalp discomfort at the stimulation site, lightheadedness, and spasms, twitching, or tingling of facial muscles. Your doctor can adjust the stimulation level throughout treatment to reduce these symptoms or suggest taking an over-the-counter pain relief medication before undergoing the procedure.
Serious side effects in TMS treatment for depression are uncommon but may include seizures, hearing loss due to inadequate ear protection, or mania in people with bipolar disorder. Seizures are rare, with an estimated risk at around 1 in 10,000 patients or 1 in 30,000 treatments. However, TMS may not be an appropriate treatment for those already at high risk for seizures, such as people with epilepsy, head injuries, or other neurologic issues. In clinical trials, less than 5 percent of patients decided to discontinue treatment because of adverse side effects. While results are promising so far, more study is required to determine if TMS may result in long-term side effects.
Does TMS Therapy Work for Depression?
Researchers conducted a six-week, randomized, double-blind study to evaluate TMS therapy’s effectiveness for treatment-resistant depression compared to a placebo. The total study population demonstrated moderate to severe unipolar, nonpsychotic major depression symptoms. Ninety-seven percent of participants experienced previous episodes of depression, had a lengthy treatment history without adequate improvement, and received an average of four previous attempts at symptom alleviation with antidepressant medication.
This study found that patients treated with TMS therapy for depression showed statistically significant response rates to treatment and remission of symptoms, around twice the rate experienced by patients treated with the placebo. In an open-label clinical trial, both study participants and researchers are aware of the treatment provided. One of these demonstrated that 50% of patients had their depression symptoms improved significantly, and 33% of patients experienced zero depression symptoms after participating in treatment for six weeks. Combining TMS with psychotherapy is the most effective treatment plan, demonstrating a response rate of 66% and a remission rate of 56% at the end of treatment.
How Does TMS Therapy Compare to ECT?
When examining the effectiveness of TMS treatment for depression, it is crucial to discuss it in comparison with ECT, the traditional treatment of choice for treatment-resistant depression and psychotic depression, and patients in need of an early response due to risk of self-harm or catatonia. A meta-analysis conducted in 2014 compared rTMS of low and high frequencies with ECT. Researchers found that ECT was superior to rTMS in regard to response and remission, and that this superiority became more pronounced among patients experiencing psychotic depression. However, patients receiving ECT were much more likely to experience cognitive side effects, especially verbal fluency and visual memory.
In patients with nonpsychotic depression, high-frequency TMS is as effective as ECT. Along with being successful at alleviating depression symptoms, TMS therapy comes with far fewer side effects than ECT. This evidence indicates that ECT will continue to be the primary treatment for severely ill patients (those experiencing psychosis, catatonia, or suicidal tendencies), but TMS is an effective option for other patients with treatment-resistant depression.
What to Expect When Undergoing TMS Therapy for Depression
During your initial visit for TMS therapy, your doctor will collect a series of measurements from your head, then use an equation to determine two specific spots on your head. The magnetic coil will be placed on your scalp over the first spot, the motor strip. A pulse of electric currents will be applied to determine the right amount of intensity, starting at a very low level and gradually increasing it until your fingers twitch. This is known as the motor threshold and will be used as a baseline for treatment, indicating how much energy will be needed for effective treatment.
After establishing this baseline, the doctor moves to the second spot, called the treatment spot, which will be the focus for the duration of your treatment at the previously determined intensity. Throughout TMS treatment for depression, the stimulation level may be changed based on your symptom relief and any side effects you experience. Your doctor will then adjust your chair to
provide you with maximum comfort. Intensity, treatment location, and chair position will be recorded and set to those specifications for subsequent treatments.
During each treatment, you will return to this chair, be given earplugs, and have the magnetic coil placed on your head. As the machine is turned on, you will feel a tapping on your forehead and hear clicking sounds. Every treatment comprises 3,000 pulses, divided into equal segments of four seconds with 40 pulses each. Between each segment is a rest period of a minimum of 10 seconds. Higher intensity thresholds mean longer treatment times and longer rest periods, but one doctor reported his typical range for treatment length as 17 minutes to 44 minutes. After each session, you may return to your normal daily activities.
TMS Results and Ongoing Treatment
Throughout therapy, TMS treatments take place every Monday through Friday for a total of six weeks. After the initial 30 sessions are completed, there are five taper sessions over the next few weeks. On the first day of treatment, and every Friday after that, you will rate your symptoms on two scales to monitor your depression level. Most patients notice signs of improvement after the first two weeks, but many report that their loved ones noticed a huge difference even before the two-week mark. Research shows that, on average, one of three patients will reach symptom remission, one will see their depression level decrease from severe to mild, and one will show no effects.
If TMS therapy improves your depression, you should discuss ongoing treatment options with your doctor. If you experience another episode of depressive symptoms, you can repeat your treatment, referred to as re-induction. TMS treatment is an intensive process showing promising results, but doctors emphasize the importance of continuing your relationship with your therapist after completing treatment.
You have seen the statistics on how TMS therapy provides a safe, effective, non-invasive solution for how to treat treatment-resistant depression. To read a personal story about how one woman’s life was completely changed by TMS therapy from Sage Clinic, click here.
Is TMS Therapy Right for You?
To be considered for TMS therapy, you must demonstrate that you have tried to alleviate your symptoms using at least one form of antidepressant medication. Many major insurance companies now include some TMS coverage, as does one plan in Medicare and one in Medicaid. However, they may require more than one failed medication for coverage eligibility. Doctors performing TMS treatment do not require a physician referral, but your insurance company may require one.
TMS is approved for patients aged 18 and older. It is not yet approved for patients with bipolar disorder. Patients with psychosis, meaning hallucinations, delusions, or suicidal thoughts, must be brought to a stable condition before beginning treatment.
Consider the following questions to see if you may benefit from TMS therapy:
Are you regularly taking medication to treat symptoms of depression?
● Do you still experience these symptoms even with medication?
● Is your medication giving you side effects?
● Have you changed medications at least one time due to these side effects?
● Does your depression interfere with your career, hobbies, or relationships?
The Future of TMS Therapy
Over the past several years, studies of TMS therapy have consistently shown promising results in alleviating the symptoms of treatment-resistant depression. Many researchers study TMS therapy as a treatment for many disorders across disciplines, hoping for insight into new methods of successfully treating patients for pain management, neurological disorders, and physical rehabilitation. Large clinical trials are currently underway to determine the effectiveness of TMS in obsessive-compulsive disorder, post-traumatic stress disorder, bipolar disorder, and pediatric depression.
Contact Sage Clinic Today to Learn More About TMS Therapy
If you or someone you love is experiencing treatment-resistant depression, contact Sage Clinic today to discuss how you can set up treatment for TMS in Albuquerque. At our interdisciplinary clinic, we focus on treating each person as a whole individual—considering all aspects of their lives when assessing their unique needs and developing the right treatment plan for them. Our collaborative, goal-oriented care is focused on the person, not the diagnosis. To find out more about our TMS treatment program, give us a call at (505) 390-1414 and see how innovative, effective, non-invasive TMS therapy can provide much-needed relief for you or your loved ones.

Founder and Clinical Director
Dr. Reuben Sutter is the founder and Medical Director for Sage Neuroscience Center. He is board-certified in general adult psychiatry and addiction medicine. He is also the past president of the psychiatric Medical Association of New Mexico. His practice focus includes severe mental illness, substance use disorders, and treatment-resistant depression. He supervises the Transcranial Magnetic Stimulation service.
Read Dr. Sutter’s Full Bio | Browse All Articles Written by Dr. Sutter